Learn how to save a life from an opioid overdose.

What is “REVIVE!”?
REVIVE! is the Opioid Overdose and Naloxone Education (OONE) program for the Commonwealth of Virginia. REVIVE! provides training on how to recognize and respond to an opioid overdose emergency using naloxone.
REVIVE! offers two types of trainings:
- Lay Rescuer trainings are between 1-1.5 hours long. This training covers understanding opioids, how opioid overdoses happen, risk factors for opioid overdoses, and how to respond to an opioid overdose emergency with the administration of Naloxone*.
- Training of Lay Rescuers prepares you to become a REVIVE! instructor. This course is 2 hours and covers the administrative requirements to lead REVIVE! trainings*.
*The basic REVIVE! Training is not sufficient for First Responders and will not qualify you for “No Cost Naloxone”. Please click the link below for information on our First Responder’s REVIVE! Training. First Responders include (Law enforcement, EMS, Fire Dept., Regional Jails, Probation and Parole, Forestry, Military, Juvenile Justice, Court Services, State Parks, and Correctional Facilities.)
First responders (law enforcement, fire, and EMS) are required to go through a separate industry specific training. Visit the First Responder Training Page for more information.
Why “REVIVE!”?
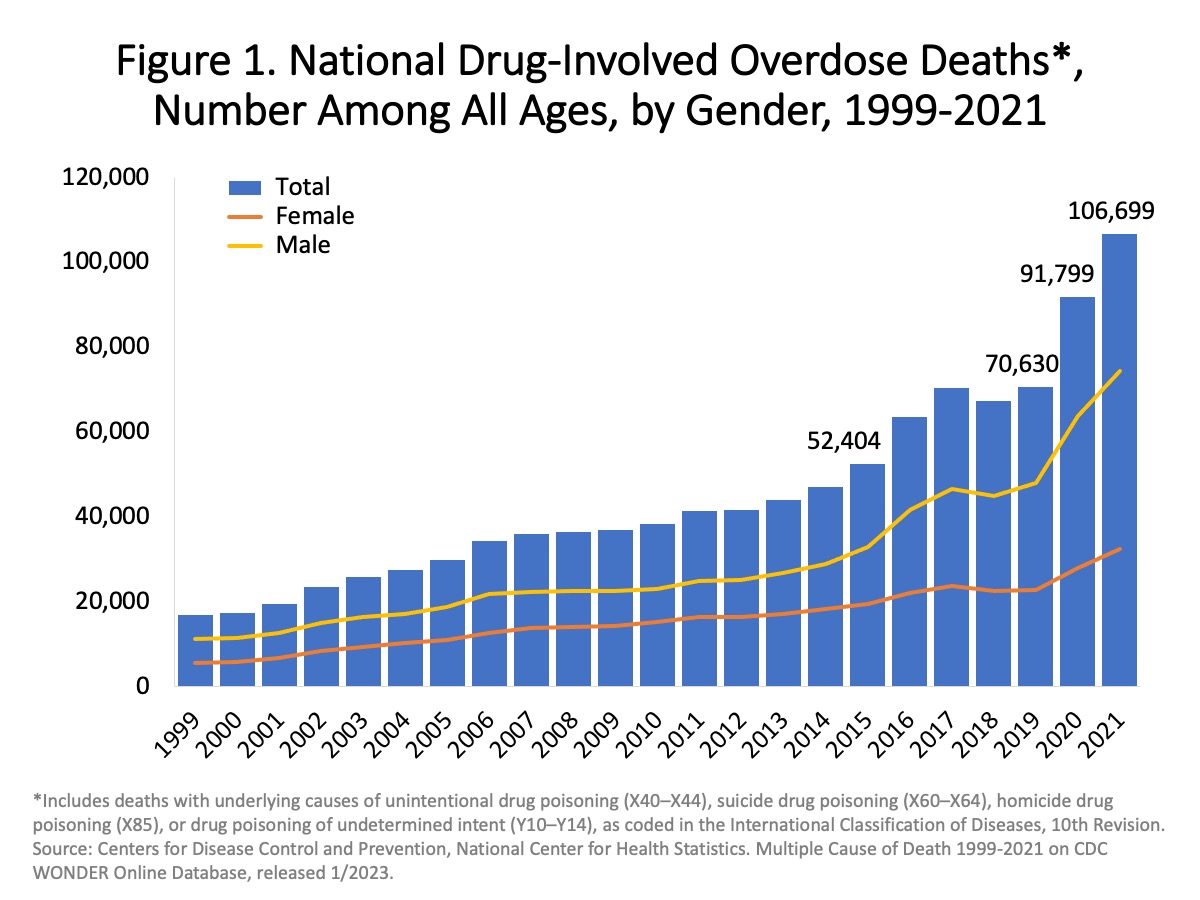
Since 2013, fatal drug overdose has been the leading method of unnatural death in Virginia, surpassing all other forms of unnatural death including homicide, suicide, motor vehicles accidents, and undetermined deaths. Opioids have been the driving force behind the large increases in fatal overdoses since 2013. In 2019, there were 1,289 deaths from all-opioids which includes all versions of fentanyl, heroin, prescription opioids and U-47700 (an illicitly manufactured synthetic opioid). (OCME Quarterly Report)
What is naloxone?
Naloxone is a prescription medicine that reverses opioid overdoses. It works by temporarily blocking the effects of opioids and helps the person to breathe again. Naloxone is the generic name but can be found under the branded name of Narcan.
How can I get naloxone?
Although naloxone is a prescription medicine, Virginia – like many states – has passed laws making it available as a standing order. The statewide standing order allows pharmacists in Virginia to dispense naloxone without requiring an individual prescription. Many community based organizations have also established a standing orders to allow community dispensing.
Anyone can access naloxone by:
- Getting a prescription from their doctor; or
- using the standing order written for the general public; or
- Virginia’s Local Health Departments and some Community Services Boards at no cost. Please call your local agency to check for availability.
- Comprehensive Harm Reduction programs
- Over-the-counter (OTC) – (summer of 2023)
For more information about the standing order, see Virginia’s Naloxone Standing Order (PDF).
Pharmacists can find more information about dispensing naloxone at the Virginia Pharmacists Association website.
The Virginia Department of Medical Assistance Services and its Medicaid health plans cover naloxone at no cost to it’s members.
REVIVE! Trainer Resources
- Lay Rescuer Training PowerPoint (updated as of February 2022) English/Spanish/Chinese
- “How-To” Guide for Trainers (updated as of April 2022) English/Spanish/Chinese
- Lay Rescuer Training Guide (updated as of April 2022) English/Spanish/Chinese
- Rapid REVIVE! Essential Talking Points(5-10 minute training) English/Spanish
- Rapid REVIVE! Handout English/Spanish
- Sign-In Sheet English/Spanish
- REVIVE! Brochure English/Spanish/Chinese
- Opioid Safety Flyer English/Spanish/Chinese
- Master Trainer Contact List (updated May 2023)
- REVIVE! Frequently Asked Questions (FAQs) (updated May 2023)
- REVIVE! Policy 2024 (January 2024)
Each time you lead a training you must complete the REVIVE! Trainer’s Report of Training: REVIVE! Trainer’s Report.
Please fill out the evaluation form: Training Evaluation
If you would like a certificate please complete a Certificate Request: REVIVE! Certificate Request
If you would like to request REVIVE! Kits, please complete the request form: REVIVE! Kits Request
Please contact Tiana Vazquez at: tiana.vazquez@dbhds.virginia.gov for any inquires about REVIVE!